Introduction
Prostatitis is a common yet often misunderstood condition affecting men’s prostate health. It involves inflammation of the prostate gland, leading to pain, urinary issues, and sexual dysfunction. This comprehensive guide explores types, causes, symptoms, and the best treatment options for prostatitis, along with expert-backed FAQs.
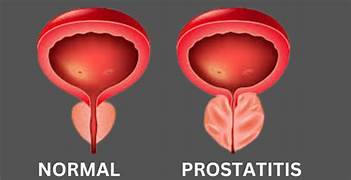
What is Prostatitis? | Types and Classifications
1. Acute Bacterial Prostatitis
Caused by bacterial infection (E. coli, Klebsiella).
Symptoms: Fever, chills, painful urination.
Requires immediate antibiotic treatment.
2. Chronic Bacterial Prostatitis
Recurring infections lasting months.
Symptoms: Pelvic pain, frequent UTIs.
Treated with long-term antibiotics.
3. Chronic Prostatitis (CPPS – Chronic Pelvic Pain Syndrome)
Most common type (90% cases).
No bacterial infection found.
Linked to nerve damage, stress, or autoimmune issues.
4. Asymptomatic Inflammatory Prostatitis
No symptoms but detected via tests.
Often found during infertility or prostate exams.
Symptoms of Prostatitis | Warning Signs
Pain: Pelvis, lower back, or genitals.
Urinary Issues: Burning sensation, frequent urination.
Sexual Dysfunction: Painful ejaculation, erectile issues.
Flu-like Symptoms: Fever (in bacterial cases).
Causes of Prostatitis | Risk Factors
Bacterial Infections (UTIs, STIs).
Pelvic Trauma (Cycling, heavy lifting).
Nerve Damage (Chronic stress, surgery).
Autoimmune Disorders (Rare cases).
Diagnosis of Prostatitis | Tests & Procedures
Digital Rectal Exam (DRE) – Checks prostate swelling.
Urine & Blood Tests – Detects infection.
Prostate Fluid Analysis – Examines bacterial presence.
Ultrasound/MRI – Rules out tumors or abscesses.
Best Treatment Options for Prostatitis
1. Antibiotics (For Bacterial Cases)
Ciprofloxacin, Levofloxacin (4-6 weeks course).
Trimethoprim-sulfamethoxazole (Chronic cases).
2. Alpha-Blockers (For Urinary Symptoms)
Tamsulosin, Alfuzosin – Relaxes prostate muscles.
3. Anti-Inflammatory Medications
Ibuprofen, Naproxen – Reduces pain and swelling.
4. Physical Therapy (For CPPS)
Pelvic floor exercises – Eases muscle tension.
5. Natural Remedies & Lifestyle Changes
Warm sitz baths – Reduces pelvic pain.
Avoid spicy/alcoholic foods – Prevents irritation.
Stress management (Yoga, meditation).
Related Keywords & Their Overview
1. Benign Prostatic Hyperplasia (BPH)
Non-cancerous prostate enlargement, different from prostatitis.
2. Prostate Massage Therapy
Controversial but helps some with chronic prostatitis.
3. UTI vs Prostatitis
UTIs affect the bladder, while prostatitis targets the prostate.
4. Prostatitis Diet
Foods like tomatoes (lycopene), green tea, and pumpkin seeds help.
FAQs (Frequently Asked Questions)
1. What is the fastest way to cure prostatitis?
Antibiotics for bacterial cases; pain relievers and lifestyle changes for CPPS.
2. Can prostatitis go away on its own?
Acute cases may improve, but chronic prostatitis often needs treatment.
3. Is prostatitis an STD?
No, but some STIs (like chlamydia) can trigger it.
4. Does prostatitis affect fertility?
Chronic inflammation may lower sperm quality.
5.What is the best treatment for bacterial prostatitis?
Antibiotics like Ciprofloxacin or Levofloxacin for 4-6 weeks are most effective.
6. Can chronic prostatitis be cured completely?
While some cases resolve, chronic prostatitis (CPPS) may require long-term management.
7. How long does prostatitis treatment take?
Acute bacterial: 2-4 weeks.
Chronic bacterial: 4-12 weeks.
CPPS: Months to years (symptom-focused).
8. Are natural remedies effective for prostatitis?
Yes! Quercetin, saw palmetto, and pelvic floor therapy help some men.
9. What antibiotics treat prostatitis?
First-line: Fluoroquinolones (Ciprofloxacin).
Alternatives: Doxycycline, Trimethoprim-sulfamethoxazole.
10. Can prostatitis cause erectile dysfunction (ED)?
Yes, due to pain or inflammation, but it’s usually temporary.
11. Is prostate massage helpful for prostatitis?
Controversial—may help chronic cases by draining fluids, but not for bacterial types.
12. Does stress worsen prostatitis?
Yes! Stress tightens pelvic muscles, aggravating CPPS.
13. Can prostatitis return after treatment?
Bacterial prostatitis can recur; CPPS often flares under stress.
14. What foods should I avoid with prostatitis?
Spicy foods
Caffeine
Alcohol
Acidic foods (tomatoes, citrus).
15. How do I relieve prostatitis pain at home?
Warm sitz baths
Over-the-counter NSAIDs (Ibuprofen)
Pelvic stretches.
16. Is prostatitis linked to prostate cancer?
No direct link, but chronic inflammation may require monitoring.
17. Can prostatitis cause infertility?
Chronic inflammation may lower sperm quality but is often reversible.
18. What’s the difference between prostatitis and UTI?
UTI: Bladder/kidney infection (more common in women).
Prostatitis: Prostate inflammation (men only).
19. Can sitting too long cause prostatitis?
Yes! Prolonged sitting (e.g., cycling) increases pelvic pressure.
20. Does ejaculation help prostatitis?
Regular ejaculation may ease congestion in non-bacterial cases.
21. What’s the role of alpha-blockers in treatment?
Drugs like Tamsulosin relax prostate muscles, improving urine flow.
22. Can prostatitis cause blood in semen?
Rarely, but inflammation may lead to hematospermia.
23. Is prostatitis contagious?
No, unless caused by an STI (e.g., chlamydia).
24. Can yoga help prostatitis?
Yes! Poses like child’s pose relax the pelvic floor.
25. Why is prostatitis so hard to diagnose?
Symptoms mimic BPH, UTIs, or interstitial cystitis. Tests like EPS help.
26. Can antibiotics fail to treat prostatitis?
Yes, if bacteria are antibiotic-resistant or it’s non-bacterial (CPPS).
27. What’s the success rate of prostatitis treatment?
Acute bacterial: 60-90% cure.
Chronic cases: 30-50% symptom relief.
28. Does prostatitis increase PSA levels?
Yes, inflammation can elevate PSA, mimicking cancer.
29. Can constipation worsen prostatitis?
Yes! Straining increases pelvic pressure.
30. Is surgery ever needed for prostatitis?
Rarely—only for abscesses or severe blockages.
31. Can probiotics help prostatitis?
Possibly, by improving gut and urinary microbiome.
32. How does chronic prostatitis affect mental health?
Chronic pain can lead to anxiety or depression—therapy helps.
33. Can drinking more water help prostatitis?
Yes! Hydration flushes bacteria and reduces irritation.
34. Does prostatitis cause frequent urination at night?
Yes (nocturia), especially with BPH overlap.
35. Can cold weather trigger prostatitis flares?
Some men report worse symptoms in cold climates.
36. Is there a link between prostatitis and IBS?
Yes! Pelvic nerve dysfunction may connect both.
37. Can weight loss improve prostatitis symptoms?
Yes, obesity increases inflammation.
38. Are there clinical trials for new prostatitis treatments?
Research includes shockwave therapy and immunomodulators.
39. Can prostatitis cause lower back pain?
Yes, referred pain from pelvic inflammation.
40. Does caffeine irritate the prostate?
Yes, it’s a bladder stimulant—reduce intake.
41. Can herbal teas help prostatitis?
Green tea (antioxidants) and chamomile (anti-inflammatory) may help.
42. Should I avoid heavy lifting with prostatitis?
Yes, straining worsens pelvic tension.
43. Can prostatitis lead to kidney damage?
Only if untreated bacterial cases spread.
44. When should I see a urologist for prostatitis?
If symptoms last >1 month or include fever/blood in urine.
Conclusion
Prostatitis can significantly impact quality of life, but proper diagnosis and treatment can manage symptoms effectively. If you experience persistent pelvic pain or urinary issues, consult a urologist for personalized care.